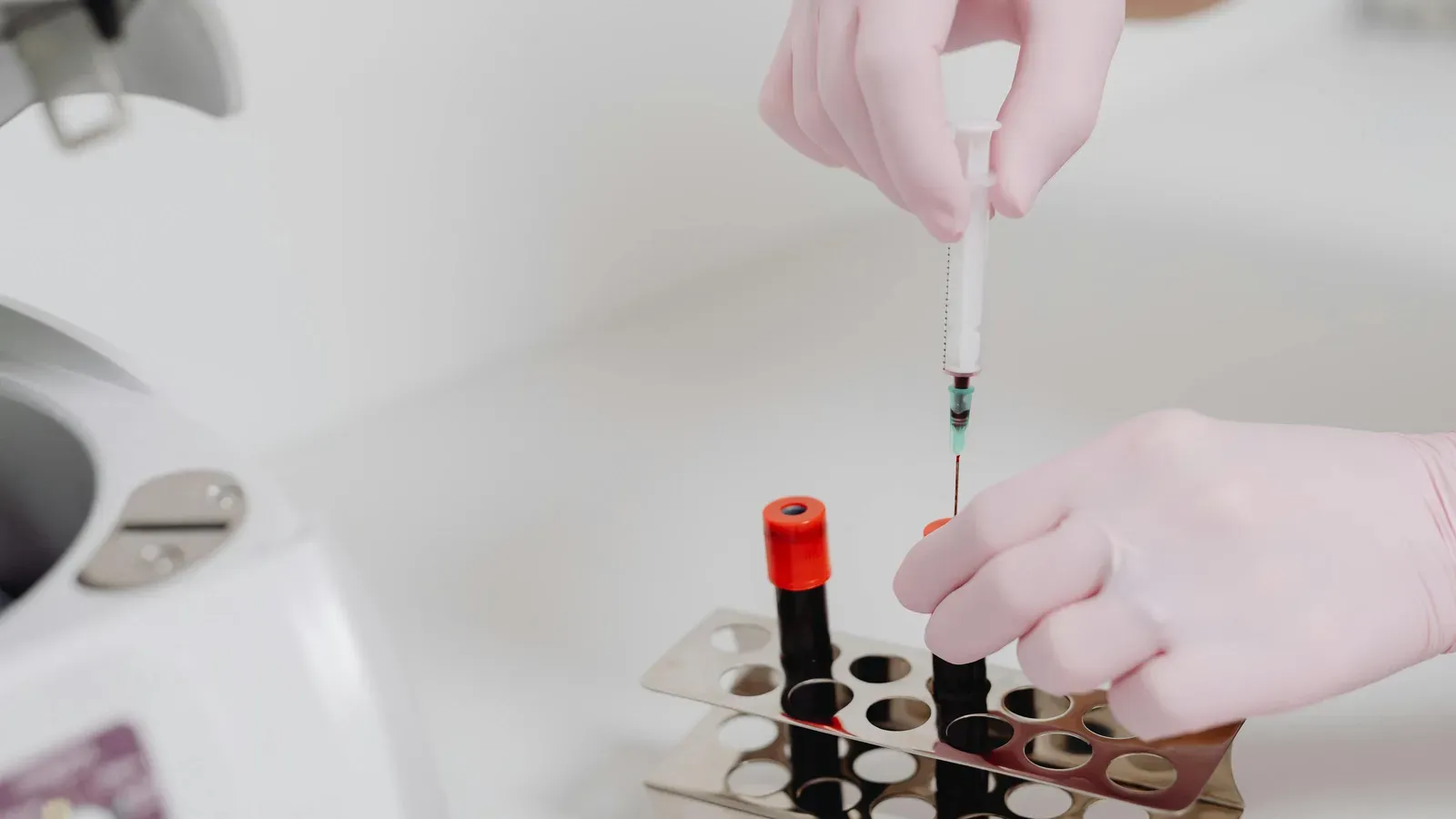
Mthfr Gene Mutation What It Means for Folate B12 and Your Health
You eat well. You take your vitamins. You do everything right—yet something still feels off. Fatigue you can't shake. Brain fog that clouds your mornings. Mood dips that don't quite make sense. What if the answer wasn't in your habits, but in your genes?
You eat well. You take your vitamins. You do everything right, yet something still feels off. Fatigue you can’t shake. Brain fog that clouds your mornings. Mood dips that don’t quite make sense. What if the answer wasn’t in your habits, but in your genes?
A common genetic variation called the MTHFR gene mutation affects roughly 40, 60% of the population, and most people have never heard of it. It doesn’t mean you’re broken. It means your body processes certain nutrients differently, and once you understand that, you can work with your biology instead of against it.
In this article, you’ll learn what the MTHFR mutation actually is, how it disrupts folate and B12 metabolism, what symptoms it can cause, and what you can do to optimize your health with this knowledge.
What Is the MTHFR Gene Mutation?
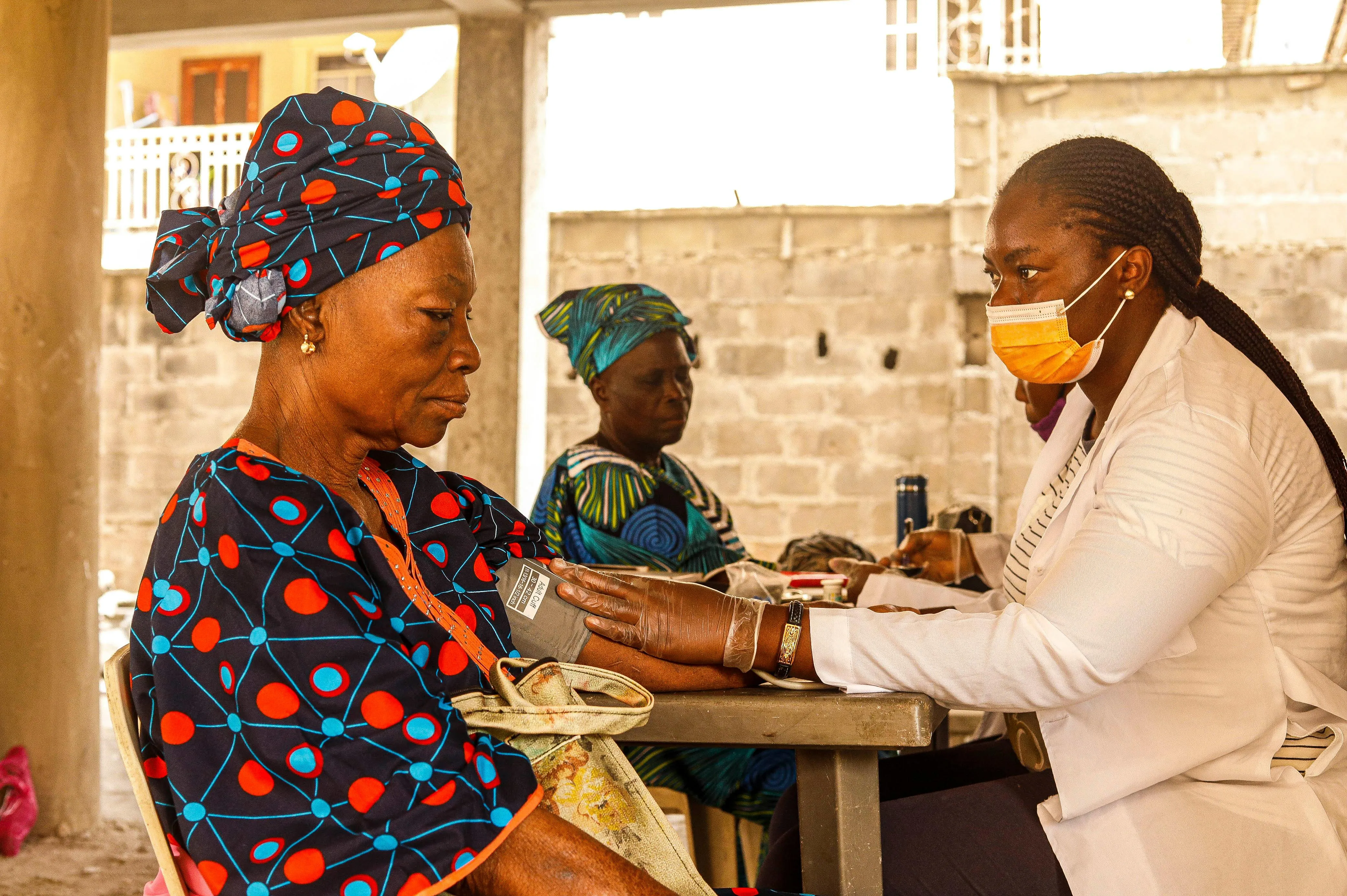
MTHFR stands for methylenetetrahydrofolate reductase. It’s a mouthful, but the concept is straightforward. This gene provides instructions for producing an enzyme that plays a central role in processing folate (vitamin B9) and regulating a process called methylation. When there’s a variant in this gene, that enzyme works less efficiently.
The two most studied variants are C677T and A1298C. The C677T variant, in particular, has been extensively researched. Carrying one copy (heterozygous) reduces enzyme activity by about 35%. Carrying two copies (homozygous) can reduce it by up to 70% [1]. That’s a significant difference in how your body handles some essential nutrients.
Having an MTHFR mutation isn’t a diagnosis or a disease. It’s a genetic variation, one that interacts with your diet, lifestyle, and environment. Understanding it gives you the power to make informed, targeted choices about your health.
How Does MTHFR Affect Folate and Methylation?

To understand why MTHFR matters, you need a quick look at methylation. Methylation is a biochemical process that happens billions of times per second in every cell of your body. It’s involved in DNA repair, detoxification, neurotransmitter production, immune function, and gene expression. It serves as your body’s master regulatory system.
The MTHFR enzyme converts folate into its active form: 5-methyltetrahydrofolate (5-MTHF). This active folate is essential for donating methyl groups throughout the body. When MTHFR isn’t working at full capacity, your cells receive less of this active folate, even if you’re eating plenty of leafy greens or taking a standard folic acid supplement [2].
What most people don’t realize is that synthetic folic acid (found in most multivitamins and fortified foods) requires conversion by the MTHFR enzyme to become usable. If your enzyme activity is reduced, unmetabolized folic acid can accumulate in your bloodstream, which research suggests may have its own downstream effects [2]. This is why the form of folate you consume matters enormously when you have an MTHFR variant.
The Link Between MTHFR, B12, and Homocysteine

MTHFR doesn’t work in isolation. It’s part of a tightly connected nutrient network that includes vitamin B12, folate, and an amino acid called homocysteine. When methylation is impaired, homocysteine (a byproduct of protein metabolism) can accumulate in the blood instead of being recycled back into beneficial compounds.
Elevated homocysteine levels are one of the most well-studied consequences of MTHFR dysfunction. Research shows that high homocysteine is associated with increased cardiovascular risk, cognitive decline, and inflammation [3]. A landmark study in Circulation found that individuals with the homozygous C677T variant had significantly higher homocysteine levels compared to those without the mutation [4].
B12 is critical in this process. Vitamin B12, specifically in its active methylcobalamin form, works alongside active folate to convert homocysteine back into methionine, a beneficial amino acid. If you’re low in B12, or if your body isn’t converting it to its active form efficiently, the entire cycle slows down. Checking both B12 and homocysteine as biomarkers gives you a far more complete picture than looking at either one alone.
What Symptoms Are Associated with MTHFR Variants?
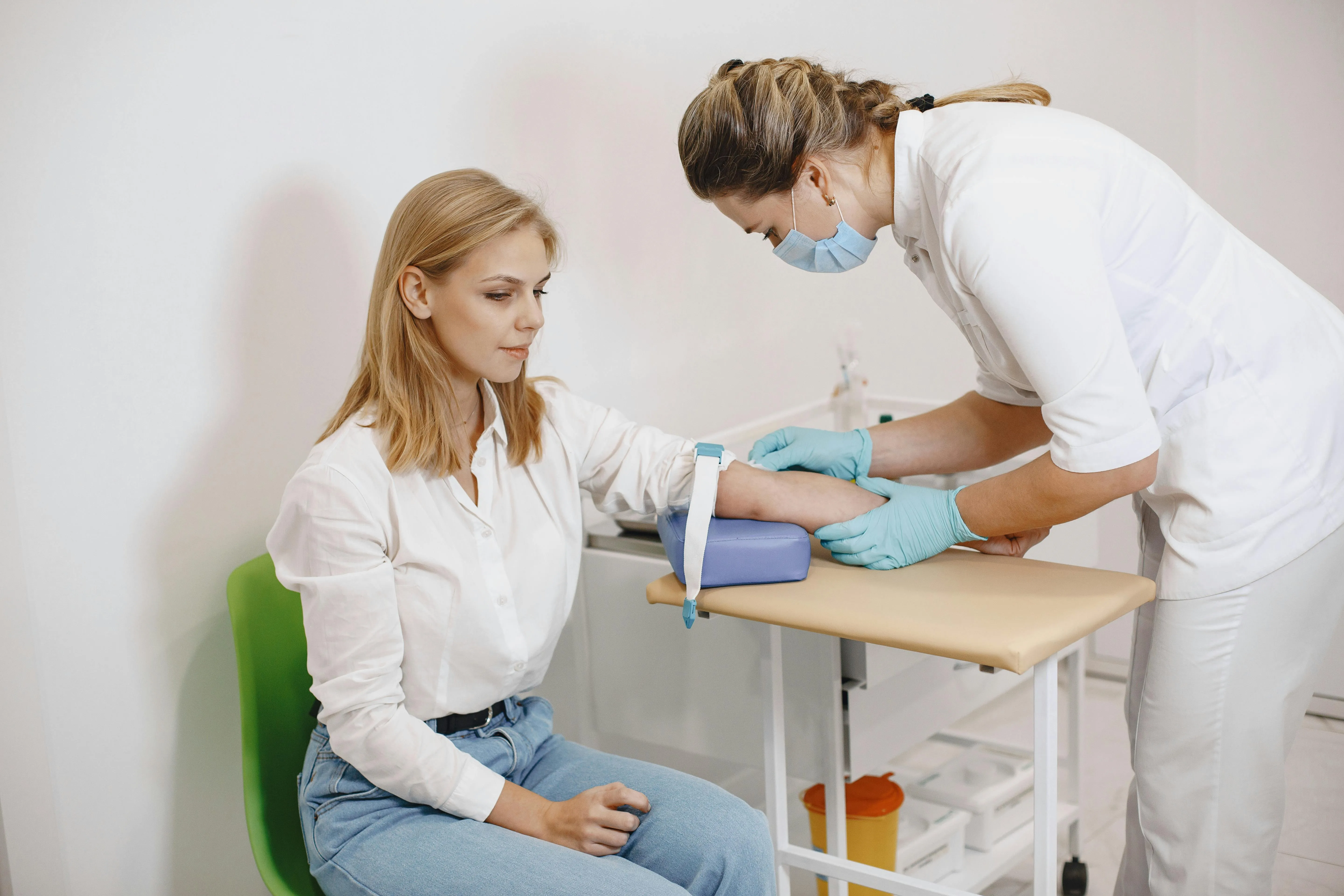
MTHFR variants don’t cause symptoms directly, but impaired methylation and elevated homocysteine can contribute to a wide range of concerns over time. Because methylation touches so many systems, the effects can feel diffuse and hard to pin down. That’s often why it goes unrecognized for years.
Common experiences reported by people with MTHFR variants include:
-
Persistent fatigue that doesn’t improve with rest
-
Brain fog, difficulty concentrating, or memory lapses
-
Mood imbalances, including anxiety or low mood
-
Sensitivity to alcohol or certain medications
-
History of pregnancy complications or recurrent miscarriage
-
Slow recovery from illness or high susceptibility to infections
These symptoms have many possible causes. An MTHFR variant is one piece of the puzzle, not a guaranteed explanation. But if you’ve been chasing answers without clear results, understanding your genetic profile, alongside your actual biomarker levels, can be the missing context you need.
Who Should Consider Testing for MTHFR?
MTHFR genetic testing is becoming more accessible, but it’s worth understanding what it can and can’t tell you. Knowing your variant status is useful context. But what matters more for your day-to-day health is how your body is actually functioning: your homocysteine levels, your active B12, your folate status. Genes load the gun; your environment and nutrition pull the trigger.
You might consider exploring MTHFR and related biomarkers if you:
-
Have a family history of cardiovascular disease or stroke
-
Experience unexplained fatigue, anxiety, or mood disorders
-
Are planning a pregnancy or have experienced pregnancy loss
-
Have been taking folic acid supplements without improvement
-
Have a personal or family history of neural tube defects
-
Feel “off” despite normal standard blood work results
Standard blood panels often don’t include homocysteine or active B12 measurements. You could have elevated homocysteine and impaired methylation for years without it appearing on a routine check-up. Targeted biomarker testing fills that gap.
How to Support Your Body with an MTHFR Variant
The good news? Once you understand how your MTHFR variant affects your nutrient needs, you can make precise, targeted adjustments. Small changes yield a big impact, and this is exactly the kind of optimization that makes a meaningful difference over time.
Research shows that supplementing with the active, methylated form of folate (5-MTHF) is significantly more effective than standard folic acid for people with MTHFR variants. A study in the American Journal of Clinical Nutrition found that 5-MTHF supplementation reduced homocysteine levels comparably to folic acid, but without the unmetabolized folic acid accumulation concern [5].
Key strategies to support methylation and reduce homocysteine include:
-
Switch to methylfolate (5-MTHF) instead of synthetic folic acid
-
Choose methylcobalamin (active B12) over cyanocobalamin in supplements
-
Increase dietary sources of natural folate: leafy greens, lentils, asparagus
-
Support choline intake, eggs, liver, and legumes support methylation as an alternative pathway [6]
-
Limit alcohol, which depletes folate and impairs methylation
-
Manage stress, as chronic cortisol elevation increases homocysteine production
One important caution: if you have the A1298C variant, high-dose methylfolate can sometimes cause overstimulation in sensitive individuals. Working with a care team lead familiar with MTHFR, and basing decisions on your actual biomarker data, is the most evidence-based approach. Your biology is unique, and personalized dosing matters.
The Role of Lifestyle in MTHFR Management
Genetics account for only part of the story. Epigenetics, the way your environment and lifestyle influence how genes are expressed, means you have real agency here. The same MTHFR variant can have very different effects depending on diet quality, stress levels, sleep, and physical activity.
Optimizing sleep is particularly relevant. During deep sleep, your brain’s glymphatic system clears metabolic waste, a process that depends on healthy methylation. Chronic sleep deprivation stresses the methylation cycle and can worsen homocysteine levels over time. Similarly, regular aerobic exercise has been shown to support cardiovascular health even in the presence of elevated homocysteine, providing meaningful protection while you address the root cause nutritionally.
Stress management also plays a direct biochemical role. Cortisol, your primary stress hormone, is metabolized through methylation pathways. Chronic stress increases the demand on your methylation cycle at the same time it depletes the B vitamins needed to run it. This is why people with MTHFR variants often notice that their symptoms worsen significantly during high-stress periods.
When to Test Your Biomarkers
Understanding your MTHFR gene status is a starting point. But the real clinical picture comes from measuring how your body is actually functioning. Homocysteine is the most direct functional marker of methylation efficiency; it tells you whether your folate and B12 pathways are working, regardless of what your genes say. Tracking it over time gives you objective feedback on whether your interventions are working.
A comprehensive approach would also include vitamin B12 (ideally active B12 or methylmalonic acid), red blood cell folate (more accurate than serum folate), and an inflammatory marker like hsCRP, since elevated homocysteine drives inflammation. Taken together, these biomarkers give you a precise, actionable picture of your methylation health.
Prevention over intervention is the core principle here. Catching elevated homocysteine early, before it contributes to arterial damage or cognitive changes, is far more effective than addressing consequences later. This is the essence of longevity medicine: using data to stay ahead of the curve.
Taking Control of Your Methylation Health
An MTHFR variant isn’t a sentence; it’s information. And information, in the right hands, is one of the most powerful tools for longevity you have. The people who thrive long-term aren’t the ones with perfect genetics. They’re the ones who understand their biology and make precise, consistent adjustments based on real data.
If you’ve been living with unexplained fatigue, mood struggles, or cardiovascular risk you can’t fully account for, the MTHFR pathway is worth understanding. Switch to methylated B vitamins. Eat folate-rich whole foods. Test your homocysteine. Work with care team lead who look at the full picture. Optimize from within.
Longevity isn’t just about living longer. It’s about living better. And it starts with knowing your numbers.
Frequently Asked Questions
What should I focus on first if I am reviewing Mthfr Gene Mutation What It Means for Folate B12 and Your Health?
Start with trend and context, not one isolated value. Compare this result with your recent symptoms, related markers, and any recent changes in sleep, stress, nutrition, or medication.
How often should Mthfr Gene Mutation What It Means for Folate B12 and Your Health be rechecked?
A practical interval is usually 8 to 12 weeks after a meaningful intervention. If symptoms worsen or a care team lead recommends sooner monitoring, follow that plan instead.
Can one abnormal Mthfr Gene Mutation What It Means for Folate B12 and Your Health result confirm a diagnosis?
No. A single result is a signal, not a final diagnosis. Confirmation usually requires repeat testing, related labs, and clinical interpretation.
When should I discuss this result with a care team lead immediately?
Discuss promptly if values are significantly out of range, symptoms are worsening, or you have new red-flag symptoms. Early review helps prevent delayed care.
Related Articles
Resources
-
Frosst P, et al. A candidate genetic risk factor for vascular disease: a common mutation in methylenetetrahydrofolate reductase. Nature Genetics. 1995;10(1):111, 113. PMID: 7647779
-
Wilcken B, et al. Geographical and ethnic variation of the 677C>T allele of 5,10-methylenetetrahydrofolate reductase (MTHFR): findings from over 7,000 newborns from 16 areas worldwide. J Med Genet. 2003;40(8):619, 625. PMID: 12566519
-
Selhub J. Homocysteine metabolism. Annu Rev Nutr. 1999;19:217, 246. PMID: 10448523
-
Varga EA, et al. Homocysteine and MTHFR mutations: relation to thrombosis and coronary artery disease. Circulation. 2005;111(19):e289, e293. PMID: 15883230
-
Lamers Y, et al. Supplementation with [6S]-5-methyltetrahydrofolate or folic acid equally reduces plasma total homocysteine concentrations in healthy women. Am J Clin Nutr. 2006;84(4):763, 770. PMID: 16522911
-
Obeid R. The metabolic burden of methyl donor deficiency with focus on the betaine homocysteine methyltransferase pathway. Nutrients. 2013;5(9):3481, 3495. PMID: 23571649