95% of Adults Have Epstein-Barr Virus: How it Increases Your Risk of Cancer
Up to 95% of adults have Epstein-Barr virus. Learn how it can increase your cancer risk and research-backed ways to keep minimise the chance of EBV-associated cancers.
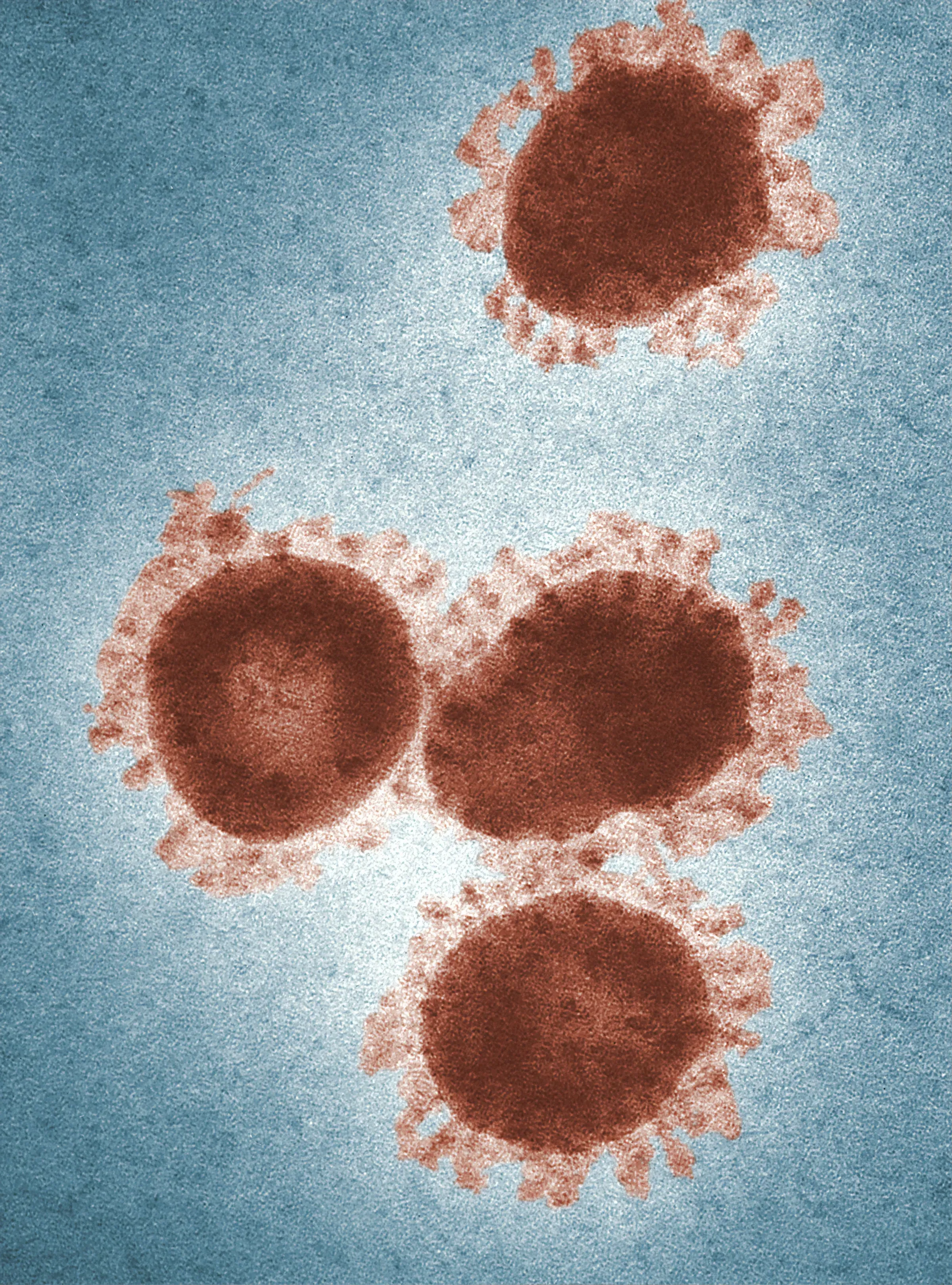
If you have ever had mono — or even if you haven’t noticed any symptoms — there is a very good chance you carry the Epstein-Barr virus. EBV infects roughly 95% of adults worldwide, making it one of the most common human viruses on the planet. For the vast majority of people, EBV quietly goes dormant after the initial infection and never causes problems again.
But for a meaningful minority, EBV can reactivate — sometimes years or decades later — leading to fatigue, immune disruption, and in rare cases, more serious health outcomes. Understanding what EBV actually does in your body, how to test for it, and when to take action puts you in control rather than in the dark.
TLDR: EBV Is Extremely Common and Usually Harmless, but Reactivation Matters
-
About 95% of adults carry EBV — most were infected in childhood without knowing it.
-
EBV goes dormant in your lymphocytes (a type of white blood cell) after the initial infection and can reactivate during periods of stress or immune suppression.
-
Specific antibody tests (VCA IgM, VCA IgG, EBNA, EA) can tell you whether you have a current, past, or reactivated infection.
-
EBV has been linked to autoimmune conditions like multiple sclerosis and lupus, chronic fatigue, and — rarely — certain cancers.
-
Evidence-based strategies including sleep, stress management, and immune support can help keep EBV in check.
What Is Epstein-Barr Virus (EBV)?
Epstein-Barr virus is a member of the herpesvirus family (human herpesvirus 4). Like other herpesviruses, EBV has a distinctive lifecycle: after the initial infection, it does not leave your body. Instead, it establishes lifelong latency inside B lymphocytes — a type of white blood cell that is part of your adaptive immune system.
EBV spreads primarily through saliva, which is why infectious mononucleosis (mono) is sometimes called the “kissing disease.” It can also spread through shared utensils, blood transfusions, and organ transplants. Most people are infected during childhood, when the virus typically causes no noticeable symptoms at all. When infection happens during adolescence or early adulthood, it is more likely to trigger mono.
The Three Phases of EBV Infection
Understanding the EBV lifecycle helps you make sense of test results and symptoms. There are three distinct phases:
1. Primary Infection
This is your first encounter with EBV. In young children, it usually passes as a mild cold or goes completely unnoticed. In teens and adults, primary infection causes infectious mononucleosis in about 25-50% of cases. Symptoms include severe fatigue, sore throat, fever, and swollen lymph nodes — and they can last weeks to months.
2. Latency
After primary infection, EBV goes dormant inside your B lymphocytes. Your immune system — particularly your lymphocytes and natural killer cells — keeps the virus suppressed. During latency, you carry the virus but have no symptoms and are generally not contagious. This is the phase most people remain in for life.
3. Reactivation
Under certain conditions, dormant EBV can “wake up” and begin replicating again. This is called reactivation. It can happen when your immune system is weakened by stress, illness, poor sleep, immunosuppressive medications, or other factors. Reactivation may be subclinical (no symptoms) or it may cause a range of issues.
Symptoms of EBV Reactivation
EBV reactivation does not always look like a full-blown case of mono. In many cases, the symptoms are subtler and can be confused with burnout, aging, or other conditions. Common signs include:
-
Persistent fatigue — the kind that does not improve with rest and feels disproportionate to your activity level
-
Sore throat — mild to moderate, sometimes recurring
-
Swollen lymph nodes — particularly in the neck and under the jaw
-
Low-grade fever — often below 100.4F (38C)
-
Muscle aches and joint pain
-
Night sweats
-
Brain fog and difficulty concentrating
If you are experiencing unexplained fatigue alongside recurrent sore throats or swollen glands, EBV reactivation is worth investigating — especially if your white blood cell count or inflammatory markers like hsCRP are abnormal.
EBV Testing: What Each Antibody Tells You
EBV testing is not a single test — it is a panel of antibody tests that together paint a picture of where you stand. Here is what each one means:
VCA IgM (Viral Capsid Antigen IgM)
This antibody appears early during a primary EBV infection and usually disappears within 4-6 weeks. A positive VCA IgM means you likely have a current or very recent active infection. If you are experiencing mono-like symptoms, this is the test that confirms acute EBV.
VCA IgG (Viral Capsid Antigen IgG)
VCA IgG develops during the acute phase but remains positive for life. A positive result simply means you have been infected with EBV at some point — which is true for about 95% of adults. On its own, a positive VCA IgG does not indicate an active problem.
EBNA IgG (Epstein-Barr Nuclear Antigen IgG)
EBNA antibodies develop 2-4 months after primary infection and persist for life. A positive EBNA IgG with a positive VCA IgG and negative VCA IgM is the classic profile of past infection with established latency — the most common and generally reassuring result.
EA IgG (Early Antigen IgG)
This is the reactivation marker. EA IgG appears during active viral replication. While it can be present during primary infection, its presence in someone with established latency (positive VCA IgG, positive EBNA) suggests the virus has reactivated. About 20-25% of healthy EBV carriers may have detectable EA IgG at any given time, so interpretation should always consider symptoms and clinical context.

How to Read Your Results
Here is a quick interpretation guide:
-
Never infected: All antibodies negative
-
Acute infection: VCA IgM positive, VCA IgG positive or rising, EBNA negative
-
Past infection (latent): VCA IgM negative, VCA IgG positive, EBNA positive — this is the most common result
-
Possible reactivation: VCA IgM negative, VCA IgG positive, EBNA positive, EA IgG positive — especially with symptoms
EBV and Autoimmune Disease: What the Research Shows
One of the most significant developments in EBV research is the growing evidence linking the virus to autoimmune conditions. This does not mean EBV causes autoimmune disease in everyone who carries it — remember, 95% of adults have EBV — but it does appear to be a contributing factor in genetically susceptible individuals.
Multiple Sclerosis (MS)
A landmark 2022 study published in Science followed over 10 million US military personnel and found that EBV infection increased the risk of developing MS by 32-fold. The study, led by Bjornevik and colleagues, showed that MS risk was extremely low among the small number of individuals who remained EBV-negative, and that seroconversion (becoming EBV-positive) preceded MS onset in virtually all cases (Bjornevik et al., 2022, PMID: 35025605). This does not mean everyone with EBV will develop MS — the absolute risk remains low — but it establishes EBV as a necessary (though not sufficient) factor.
Lupus and Other Autoimmune Conditions
A 2020 review by Houen and Trier examined the evidence linking EBV to multiple autoimmune diseases, including systemic lupus erythematosus (SLE), rheumatoid arthritis, and Sjogren’s syndrome. The proposed mechanism involves molecular mimicry — EBV proteins resemble human proteins closely enough that the immune system may begin attacking the body’s own tissues (Houen & Trier, 2020, PMID: 32120399). If you have a family history of autoimmune disease, keeping your immune system well-supported may be particularly important for managing latent EBV.
Chronic Fatigue Syndrome (ME/CFS)
The relationship between EBV and chronic fatigue syndrome has been debated for decades. Current evidence suggests that EBV reactivation may trigger or perpetuate ME/CFS in a subset of patients, particularly those whose initial mono was severe. If you have been dealing with unexplained fatigue lasting more than six months, asking your care team lead about EBV reactivation testing (particularly EA IgG) is reasonable. Monitoring your overall immune health through markers like your white blood cell count can provide additional context.
EBV and Long COVID
An emerging area of research suggests that EBV reactivation may play a role in long COVID symptoms. A 2021 study by Gold and colleagues found that 73% of long COVID patients had positive EA IgG (indicating EBV reactivation), compared to only 10% of controls who had recovered from COVID without lingering symptoms (Gold et al., 2021, PMID: 34375979).
The hypothesis is that SARS-CoV-2 infection may weaken immune surveillance enough to allow dormant EBV to reactivate, and this reactivation may contribute to the fatigue, brain fog, and other symptoms characteristic of long COVID. While more research is needed to establish causation, this finding suggests that EBV testing could be valuable for people experiencing persistent post-COVID symptoms.
EBV and Cancer Risk: Rare but Real
It is important to be transparent about the fact that EBV is associated with certain cancers. However, context matters enormously here. Billions of people carry EBV, and the vast majority never develop an EBV-associated malignancy. The cancers linked to EBV include:
-
Nasopharyngeal carcinoma — most common in southern China and Southeast Asia, with genetic and environmental co-factors playing major roles
-
Burkitt’s lymphoma — primarily seen in equatorial Africa, often in conjunction with malaria co-infection
-
Hodgkin’s lymphoma — EBV is detected in tumor cells in about 30-50% of cases in developed countries
-
Post-transplant lymphoproliferative disorder — occurs in immunosuppressed organ transplant recipients
The common thread in EBV-associated cancers is prolonged immune suppression or specific genetic susceptibility — not EBV infection alone. Maintaining robust immune function through the strategies outlined below is one of the best ways to minimize this already-low risk. Keeping an eye on your white blood cell count and inflammatory markers can help you and your care team lead catch immune changes early.
Evidence-Based Strategies for Managing EBV
Whether you are dealing with known EBV reactivation or simply want to keep the virus dormant, these strategies are supported by research and clinical practice:
Prioritize Sleep
Sleep is when your immune system does its most important maintenance work. During deep sleep, your body produces cytokines — proteins that help fight infection and inflammation. Chronic sleep deprivation reduces natural killer cell activity, which is critical for keeping EBV suppressed. Aim for 7-9 hours per night and maintain a consistent sleep schedule.
Manage Stress
Chronic psychological stress is one of the most well-documented triggers for EBV reactivation. Stress hormones like cortisol suppress the very immune cells responsible for keeping EBV in check. Evidence-based stress reduction includes regular physical activity, mindfulness meditation, time in nature, and maintaining social connections. If stress is chronic and unmanageable, professional support from a therapist is not a luxury — it is a health intervention.
Support Your Immune System Nutritionally
Several nutrients play direct roles in antiviral immune function:
-
Vitamin D — low vitamin D levels are associated with increased susceptibility to viral infections and autoimmune disease. If you are not getting regular sun exposure, testing and supplementation are worth considering. Learn more about raising your vitamin D levels naturally or explore practical steps to improve your vitamin D.
-
Zinc — essential for T-cell function and natural killer cell activity. Good dietary sources include oysters, red meat, pumpkin seeds, and lentils. Supplementation (15-30 mg/day) may help if dietary intake is insufficient.
-
Selenium — supports antioxidant defenses and immune regulation. Brazil nuts are an exceptionally rich source (1-2 per day provides adequate selenium).
-
Vitamin C — supports white blood cell function and acts as an antioxidant. Aim for adequate intake through fruits and vegetables, with supplementation (500-1000 mg/day) as a reasonable addition during periods of immune stress.
Exercise — But Don’t Overdo It
Moderate, regular exercise enhances immune surveillance and reduces inflammation. However, overtraining or intense exercise during active reactivation can worsen symptoms and further suppress immunity. If you are recovering from EBV reactivation, start with walking, gentle yoga, or light resistance training and gradually increase intensity as your energy returns.
Reduce Alcohol and Quit Smoking
Both alcohol and tobacco suppress immune function. Alcohol in particular disrupts the gut microbiome and impairs the function of immune cells in the mucous membranes — your first line of defense. If you are managing EBV, limiting alcohol to a few drinks per week (or less) and avoiding tobacco entirely are straightforward wins.
When to See a care team lead
Most people with latent EBV do not need medical intervention. However, you should consult a care team lead if you experience:
-
Persistent fatigue lasting more than 2-3 weeks that does not improve with rest
-
Recurrent sore throats with swollen lymph nodes
-
Unexplained low-grade fevers
-
Symptoms consistent with autoimmune disease (joint pain, rashes, numbness)
-
Night sweats or unexplained weight loss
Your care team lead can order an EBV antibody panel, check your white blood cell count and differential, and assess inflammatory markers to determine whether EBV reactivation or another condition is responsible for your symptoms.
Frequently Asked Questions
Can EBV come back?
Yes. Once you are infected with EBV, the virus remains in your body for life in a dormant state. It can reactivate during periods of immune suppression — from chronic stress, illness, poor sleep, or immunosuppressive medications. Reactivation is usually milder than the original infection, and many people experience subclinical reactivation (detectable on blood tests but without noticeable symptoms).
Is EBV the same as mono?
Not exactly. EBV is the virus; infectious mononucleosis (mono) is a disease that EBV can cause. Most people who are infected with EBV — especially those infected in early childhood — never develop mono. Mono tends to occur when primary EBV infection happens during adolescence or adulthood. You can have EBV without ever having had mono.
How do I know if my EBV is reactivated?
The most reliable way is through blood testing. An EBV antibody panel that shows positive EA IgG (Early Antigen) alongside positive VCA IgG and EBNA IgG suggests reactivation in someone with established latent infection. Symptoms like unexplained fatigue, sore throat, and swollen lymph nodes provide clinical context, but the blood test is what confirms reactivation.
Can EBV be cured?
There is currently no cure for EBV — once infected, you carry the virus for life. Antiviral medications like valacyclovir can reduce active viral replication during acute infection or reactivation, but they do not eliminate the dormant virus. The goal of management is to keep EBV in latency through immune support. Several EBV vaccine candidates are in development, but none are currently approved.
Should I get tested for EBV?
Testing makes sense if you are experiencing symptoms that could indicate reactivation (persistent fatigue, recurrent sore throat, swollen glands), if you have an autoimmune condition and want to understand contributing factors, or if you are dealing with long COVID symptoms. For most healthy adults without symptoms, routine EBV screening is not necessary — a positive VCA IgG (which 95% of adults will have) simply confirms past exposure and is not actionable on its own.
The Bottom Line
Epstein-Barr virus is one of the most successful human pathogens in history — precisely because it has evolved to coexist with us quietly. The vast majority of people who carry EBV will never have a problem with it. But if you are experiencing unexplained fatigue, immune dysfunction, or symptoms that do not add up, EBV reactivation deserves a spot on your investigation list.
The science is clear: keeping your immune system strong through adequate sleep, stress management, good nutrition, and regular exercise is the single best strategy for keeping EBV dormant. And if you suspect reactivation, a simple antibody panel can give you and your care team lead the information you need to take action.
Related Articles
Resources
-
Bjornevik K, Cortese M, Healy BC, et al. Longitudinal analysis reveals high prevalence of Epstein-Barr virus associated with multiple sclerosis. Science. 2022;375(6578):296-301. PMID: 35025605
-
Houen G, Trier NH. Epstein-Barr Virus and Systemic Autoimmune Diseases. Front Immunol. 2020;11:587380. PMID: 32120399
-
Gold JE, Okyay RA, Licht WE, Hurley DJ. Investigation of Long COVID Prevalence and Its Relationship to Epstein-Barr Virus Reactivation. Pathogens. 2021;10(6):763. PMID: 34375979
-
Centers for Disease Control and Prevention. Epstein-Barr Virus and Infectious Mononucleosis. cdc.gov/epstein-barr
-
Fugl A, Andersen CL. Epstein-Barr virus and its association with disease. J Pathol. 2019;248(3):346-362. PMID: 30714131